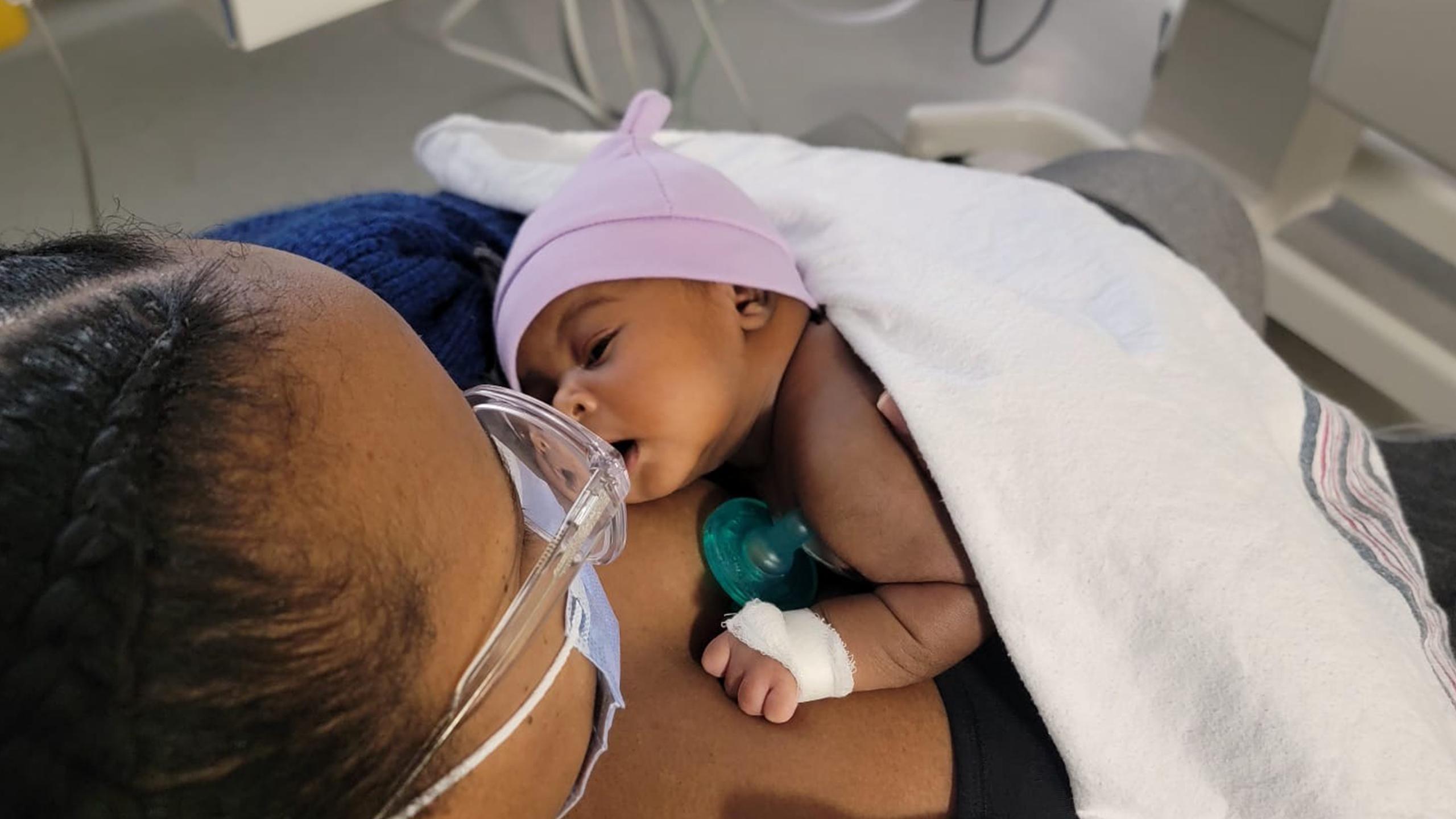
Toronto mother finds life‑saving support through Sinai Health’s high‑risk pregnancy program

When Stacee Samuels discovered she was pregnant, joy quickly gave way to worry.
She knew that several factors placed her pregnancy in the high-risk category. She was older, had a high body mass index, and was aware of troubling statistics about complications experienced by Black mothers.
“I was nervous,” Stacee recalls. “You hear all the statistics about maternal health outcomes, and I didn’t know what my journey would look like.”
Her physician referred her to Sinai Health’s Medical Disorders of Pregnancy (MDP) program at The Frances Bloomberg Centre for Women’s and Infants’ Health, where specialists care for patients whose pregnancies are complicated by existing medical conditions or emerging health risks.
There, Stacee met Dr. Kristin Harris, a maternal-fetal medicine specialist and head of the Medical Disorders of Pregnancy program.
How Sinai Health bridges medical complexity and pregnancy care
Dr. Harris and her colleagues care for patients whose pregnancies may be affected by a range of medical factors, including diabetes, inflammatory bowel disease, hypertension and other chronic health conditions. They also support individuals who enter pregnancy with additional considerations — such as age or body size — that can influence how their care is planned. These factors often exist long before pregnancy begins and can become more complicated as pregnancy progresses.
“Pregnancy isn’t a single event,” Dr. Harris explains. “It’s layered on top of a person’s existing health, social circumstances and access to care.”
Her team’s role is to recognize risks early and plan carefully — monitoring both mother and baby while coordinating care with specialists across disciplines.
At Sinai Health, that collaboration is central to the program’s success. Obstetricians, anesthesiologists, internists, endocrinologists, neonatologists and nurses work together to anticipate potential complications and respond quickly when conditions change.
For Stacee, that coordinated approach was reassuring from the very beginning.
“I went into my first appointment with Dr. Harris ready to advocate for myself,” she says. “But she took the time to walk through my questions and explain the risks and how they could be managed. That was the first time I really understood what patient-centred care meant.”
Much of Stacee’s pregnancy progressed smoothly. Her care plan included close monitoring to track her baby’s growth and watching for changes in Stacee’s health.
But as her due date approached, her blood pressure began to rise — a warning sign of pre-eclampsia, a potentially life-threatening condition that can develop rapidly in pregnancy. The team admitted Stacee to the Hospital and monitored both her and the baby closely. Ultrasound revealed concerning changes.
“A pregnancy can appear stable for long periods, but that stability can change quickly,” says Dr. Harris. “That’s why these pregnancies require specialized, coordinated care so we can recognize those changes and respond right away.”
Right before Stacee’s planned delivery, her condition became even more complicated. Her platelet levels — critical for blood clotting — had dropped dramatically, requiring the involvement of multiple medical specialties to safely deliver her baby.
Just after midnight on January 1, the care team moved forward with delivery. Her daughter, Kaiya, became Mount Sinai Hospital’s first baby of 2025.

Responding quickly when a baby needs immediate, advanced care
While Kaiya’s arrival was joyful, the days that followed were filled with uncertainty.
Shortly after her birth, doctors discovered that she had experienced a bilateral brain bleed — a serious condition that can occur in premature or medically fragile newborns. Kaiya was admitted to the Newton Glassman Charitable Foundation Neonatal Intensive Care Unit (NICU) for specialized care.
“It was all a blur,” Stacee remembers. “I didn’t hold her until hours after she was born. She went straight to the NICU, and we were so worried.”
The neonatal team monitored Kaiya closely and provided the treatments she needed. Meanwhile, Stacee recovered with the support of the same care team that had guided her pregnancy. Kaiya had to spend 10 days in the NICU before she was cleared to go home.
For Stacee, what stood out most was how seamlessly the team worked together.
“I felt like a minor hospital celebrity. I saw so many specialists, but every doctor already knew my case,” she says. “Dr. Harris had spoken with them beforehand, so I never had to start from scratch explaining my situation.”
For Dr. Harris, compassionate care is as important as clinical expertise. “It means listening without rushing and giving patients the space to process information and ask questions,” she says. “Pregnancy can carry both medical risk and emotional weight.”
That compassion made a profound difference for Stacee during the most difficult moments of her pregnancy.
“Dr. Harris is incredibly smart, but she’s also deeply empathetic,” Stacee says. “She anticipates how a patient might feel and makes sure you understand what’s happening.”

Why continued funding matters for the future of family care
Today, Kaiya is thriving.
Just over a year old, she is walking, babbling and meeting every developmental milestone. “She’s doing everything a child her age should be doing,” Stacee says proudly. “I couldn’t imagine life without her.”
Looking back, Stacee says access to specialized care made all the difference. “It’s life-saving for both the parent and the baby,” she says. “Knowing that I was in the best possible hands, and that my daughter was in the best possible hands, really made a difference during such a difficult period.”
Programs like Sinai Health’s Medical Complications in Pregnancy program depend on the collaboration of highly specialized teams, advanced monitoring technologies and continuous research to improve outcomes for families facing complex pregnancies. They also provide an essential training ground for the next generation of physicians to learn about this highly specialized complex care and research — laying a strong foundation for future innovations.
Dr. Harris says donor support plays a critical role in making that work possible. “Community and philanthropic support allow us to develop new programs and innovative ideas that help us better support patients in pregnancy and their babies.”
You can help advance complex pregnancy care for patients like Stacee
When you give to Sinai Health, you become part of Stacee’s story — helping deliver the care, comfort and expertise that guide families through complex pregnancies. Your support helps make sure that even in some of life’s most uncertain moments our team is able to provide innovative solutions and compassionate care. Donate today.
In addition to her gratitude to Dr. Harris for the care throughout her pregnancy, Stacee is thankful for the many other care providers at Sinai Health who supported her and Kaiya. Especially: the NICU team (including Dr. Jennifer Young and nurses, Sandra and Julius), the Labour and Delivery team (including Drs. Homero Flores, Mia Kibel and Nicole Wade and nurses, Masoumeh, Gabrielle and Jasleen), postpartum nurses (Karen, Sherie and Jade), and the hematology team (Tabea Sutter and Nadine Shehata).