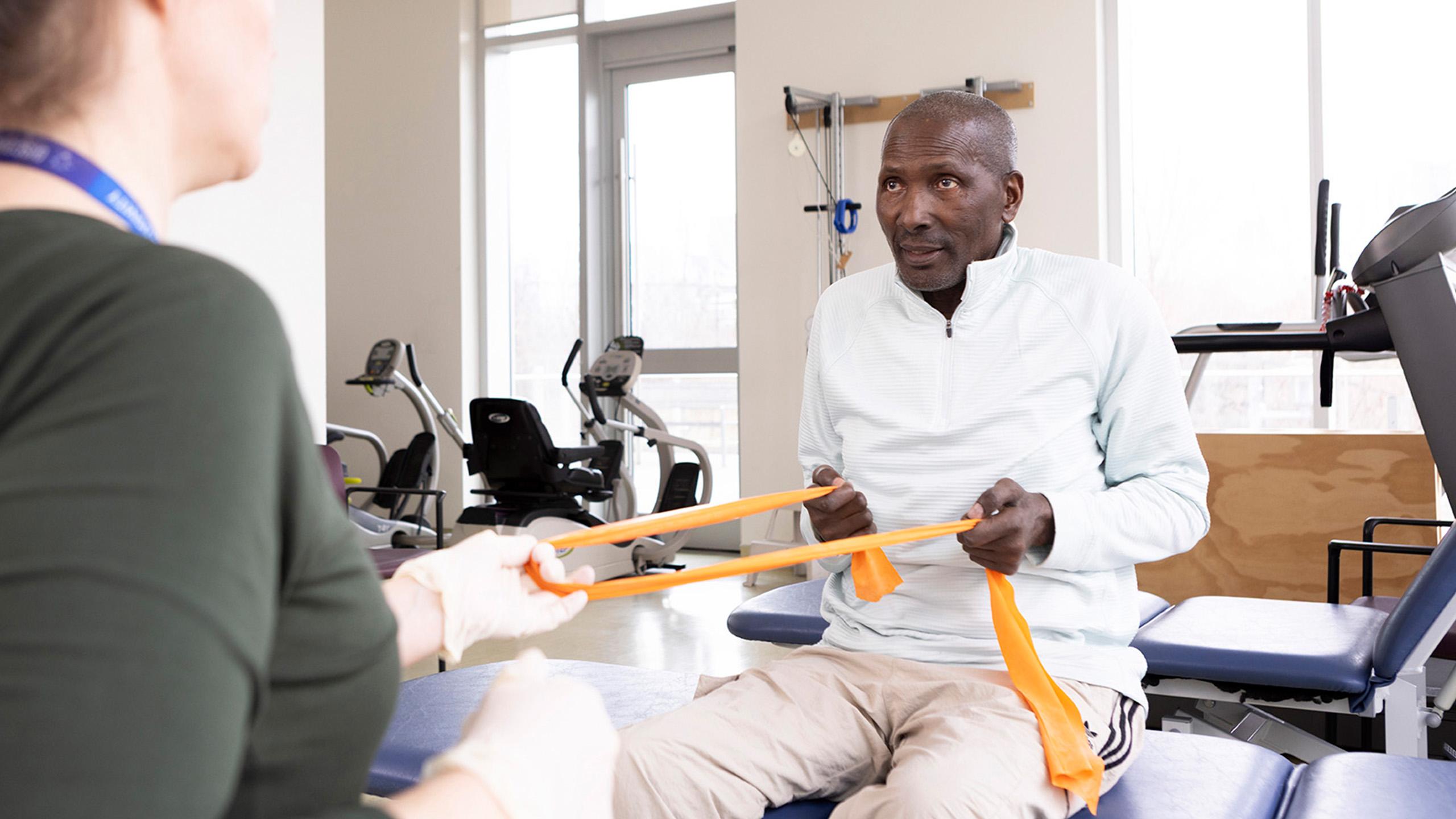
Mount Sinai Hospital’s outpatient palliative care program enhances quality of life for patients with life-limiting illnesses

In 2019, Raisy Mandel and her family found out that her mother Sheila’s breast cancer had returned. It was a shock that almost thirty years after her initial diagnosis, she now had an incurable form of the disease. At 85, Sheila was also in the early stages of dementia and she would rely on her family to help make decisions about her care.
“An oncologist in my family recommended starting palliative care right away,” says Raisy. “It was the best piece of advice I’ve ever received.”
A unique model of care
The Temmy Latner Centre for Palliative Care’s outpatient clinic supports individuals like Sheila who have a life-limiting illness. Patients are referred to the program though a Sinai Health physician. The clinic is located within the The Ruth Burnett Centre for outpatient oncology. This allows oncologists, palliative care physicians, nurses and an interprofessional care team to work together to provide a seamless care experience.
Palliative care physicians and oncologists at the clinic are often able to meet with their patients together. Dr. Harleen Toor, a physician and Medical Lead for the clinic says this unique model of care is more convenient for patients and helps them access palliative care earlier. “Regardless of where a patient is in the course of their illness, palliative care can help with managing symptoms, accessing supports and planning for the future,” says Dr. Toor “Research shows starting care earlier leads to better outcomes in meeting the needs and goals of patients and their family caregivers.
Active treatment and palliative care work together
Raisy says Dr. Toor and the entire care team have been a ‘lifeline’ for the family, answering questions and explaining treatment options. “ My father, like a lot of people, had the impression that palliative care is for people at the immediate end of life,” says Raisy. “But Dr. Toor reassured us that even though they may not be able to cure my mom’s cancer, it didn’t mean there wouldn’t be any more treatment.”
With their doctors’ advice, the family decided to move forward with radiation therapy. This would actively treat the cancer while also supporting their palliative care goals to relieve Sheila’s symptoms.
Managing pain was a priority and Raisy says “If we didn’t have Dr. Toor’s care right from the start I think my mother would have had a lot more pain.”
The treatment worked so well that Sheila was able to travel to Israel in 2019 to attend a family wedding.
Changing care goals
Patients’ needs and goals change throughout the course of their illness. Several months ago, the Mandel family went through one of these care transitions. They decided it was time to stop treatments that would prolong Sheila’s life. Raisy says Dr. Toor’s compassionate and straightforward approach helped the family to make this decision based on her mom’s wishes.
The change meant that Sheila would no longer need care from her oncologist. For the family, this care transition was easier knowing Dr. Toor would continue to provide palliative care. “For our family, going through this has been a team effort and Dr. Toor has been the leader of our team,” says Raisy.
Sheila continues to live at home and Raisy says that although she can’t predict the future, the support of Dr. Toor and the outpatient palliative care clinic is comforting. The Mandel family and the care team will continue working together to help Sheila enjoy the best-possible quality of life.