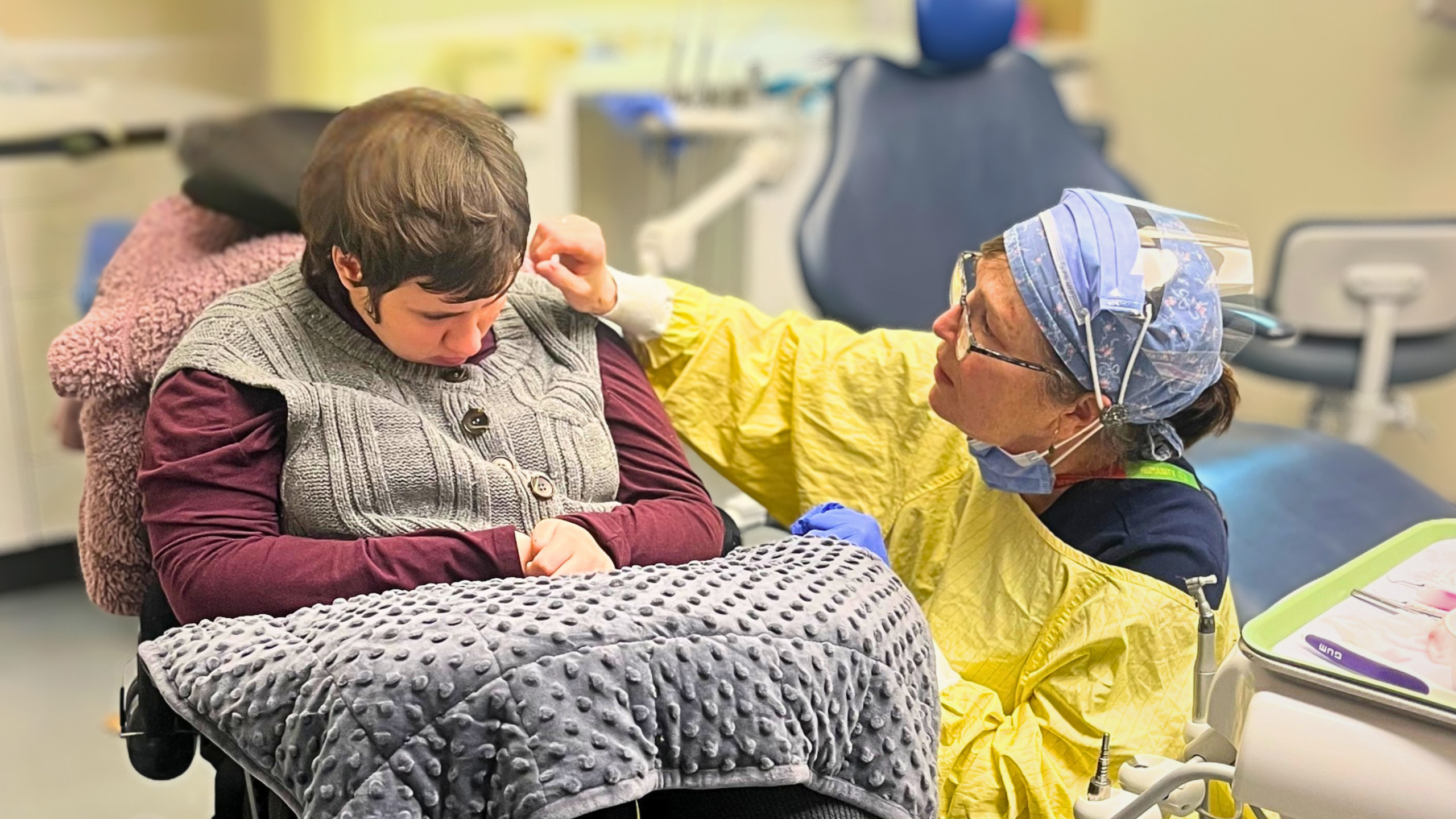
General Internal Medicine Unit provides specialized high-flow oxygen therapy for patients with COVID-19
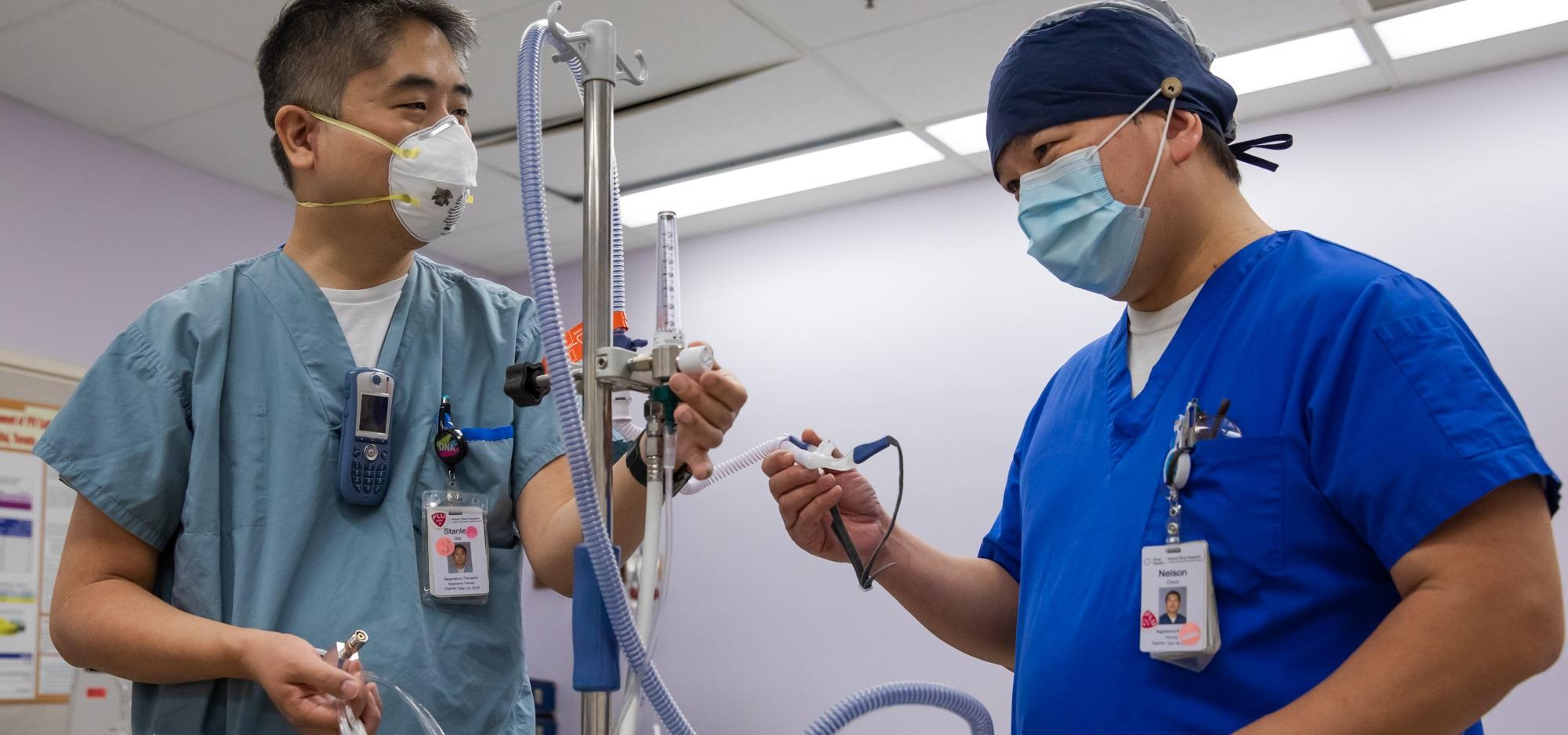
Mount Sinai’s 12 South General Internal Medicine Unit has taken on a unique role in caring for patients with severe COVID-19. Early this year, the team implemented a project to become the designated unit for patients who need high flow nasal cannula (HFNC) oxygen therapy.
Katherine McQuaid-Bascon, Senior Director, Health Disciplines, supported the interprofessional team in implementing strategies and processes to create this specialized capacity on 12 South. She says HFNC, which delivers heated, humidified oxygen at a higher flow rates, is an essential piece in the toolbox when caring for patients with COVID-19, along with treatments such as traditional oxygen therapy and mechanical ventilation.
“For some patients with COVID-19, HFNC enables them to recover when traditional oxygen therapy has not worked,” she says. “Other patients may choose HFNC because they do not want to be intubated, which is a more invasive treatment that requires admission to the intensive care unit (ICU), but they still want active medical treatment. In other cases, high flow oxygen therapy is the necessary modality to provide supplemental oxygen as they recover.”
A group of interprofessional educators and leaders from various areas including Nursing, Respiratory Therapy, Palliative Care, Rehabilitation and Biomedical Engineering led various aspects of initiative to train and equip the 12 South team to become Mount Sinai’s designated unit for HFNC patient care. “With more patients requiring this therapy due to COVID-19, cohorting these patients on one unit enables us to optimize our resources and provide the best care,” Katherine says.
Implementing this type of specialized care is not a simple task. The 12 South team participated in training sessions about the new equipment and received additional education about the specific needs of patients on HFNC. They also built connections with the Palliative Care and ICU/Access teams, working together to provide patient-centred care.
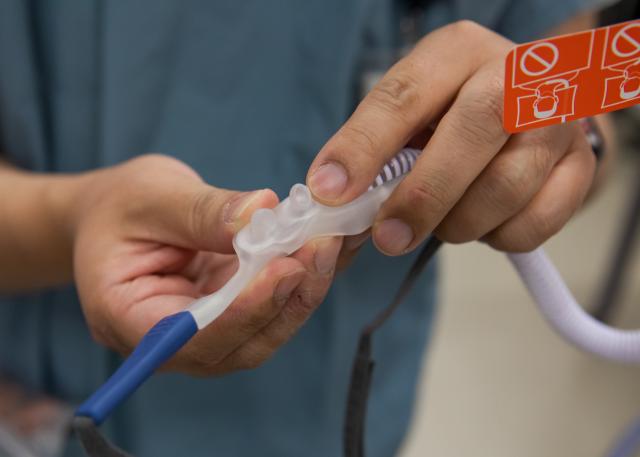
Violet McNeil, a Registered Nurse on the unit says although HFNC has been used on 12 South prior to the pandemic, there was a ‘learning curve’ adjusting to new processes, new equipment and caring for more patients with severe COVID-19. “12 South nurses are definitely a group of skilled and competent nurses,” she says. “We’ve been able to adapt to the equipment and supplies needed and are able to assess the patients according to their oxygen needs. We have had wonderful support from Respiratory Therapists who have been an integral part of this process. We’re continuing to provide the best quality patient care with evidence-based practice.”
Katherine says the teamwork on this initiative has been commendable. “This is a team that collaborates well and has great communication. In this project they showed that they’re open to new ideas, providing feedback, asking great questions and working together. All of these factors contributed to the success of this project.”
The 12 South Unit can now provide care for up to eight patients who require HFNC at a time, crucial capacity for the health care system during the third wave of COVID-19.