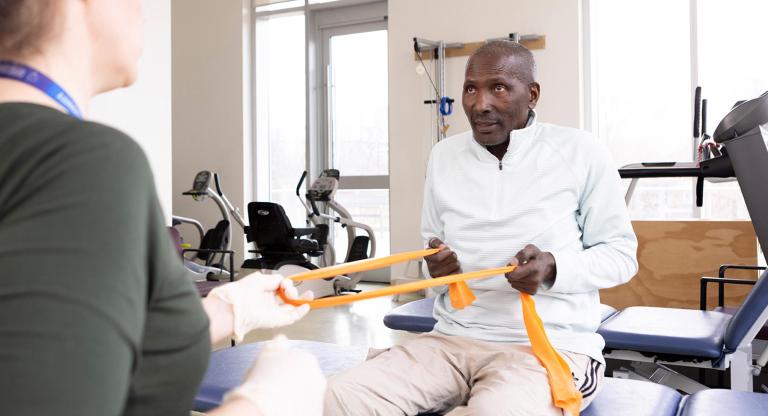
Mount Sinai Hospital teams create more critical care capacity in the third wave
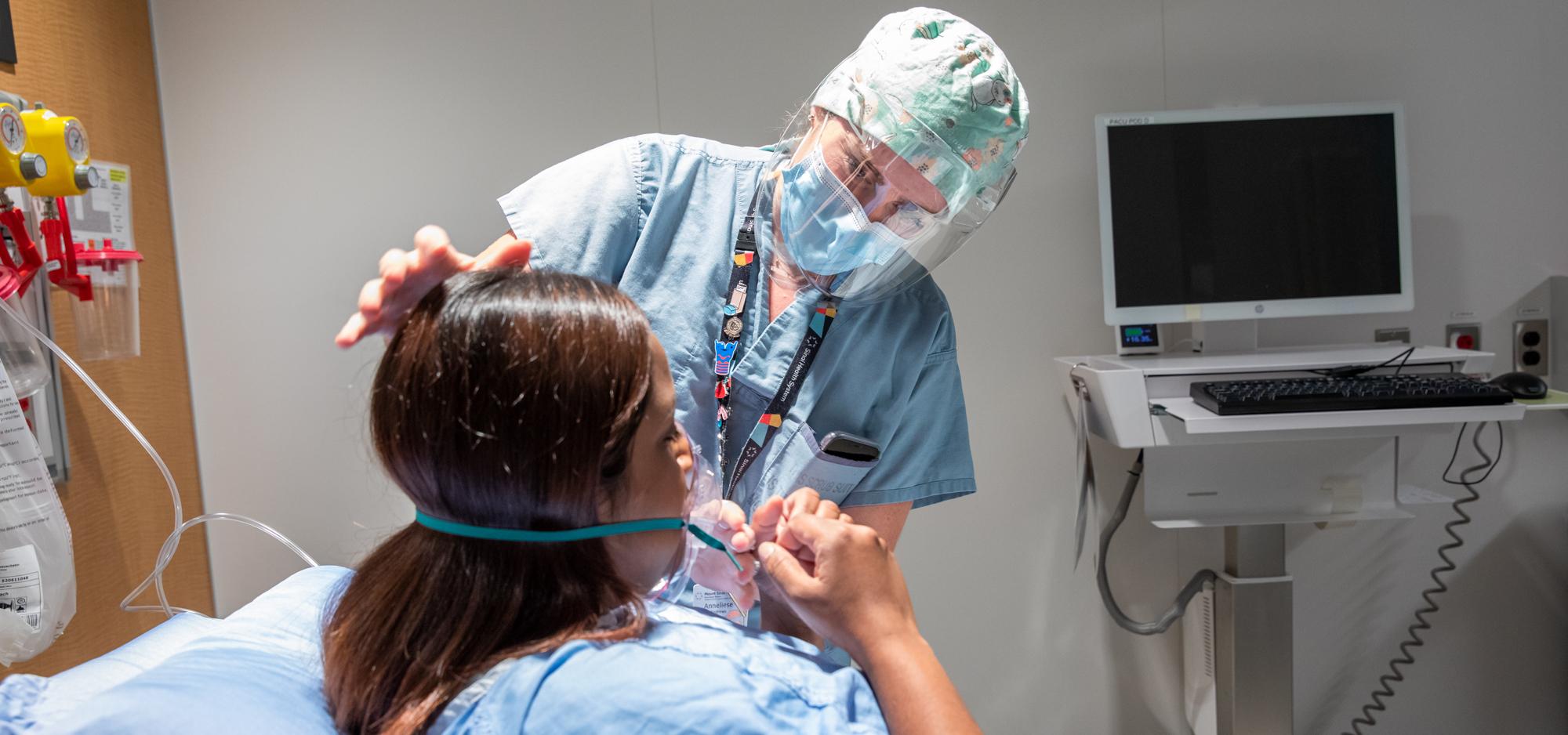
Earlier this spring, as Ontario headed into the third wave of COVID-19, many hospitals across the GTA found ways to create new critical care spaces from tents to temporary hospitals, to meet the growing need for care beds.
As the number of cases continues on a downward trend, the teams at Mount Sinai Hospital, part of Sinai Health, reflect on how they stepped up as a key system partner to create more capacity, to support GTA hospitals in COVID-19 hot spots.
Creating more capacity takes constant coordination to balance staffing, beds and equipment. It takes a very engaged group of people to make that happen.
– Carolyn Farquharson
“Our care teams went above and beyond to support greater bed capacity at our acute care campus to ensure patients would receive care and to relieve pressure on other hospitals,” says Carolyn Farquharson, Director, Patient Flow & Admitting who was also serving as the interim Senior Clinical Program Director of Urgent and Critical Care during the peaks of the second and third waves.
Through strong collaborations, and with responsive leadership providing key supports, teams expanded the Intensive Care Unit (ICU), repurposed the post-surgical recovery unit (PACU) into high-functioning Critical Care units and made medical and surgical beds available to support system-wide capacity.

“What we’ve been able to do, speaks to the resilience and flexibility of our teams to continue to provide quality patient care in this difficult circumstance. Highly trained professionals moved into different roles, in different spaces and with new patient populations,” says Lisa Wayment, Senior Clinical Program Director, Surgery and Oncology.
“Our teams responded by saying, we will step into these roles and help with this work.”
-Lisa Wayment
Teams pulled together with insights-sharing among anesthetists, ICU intensivists and General Internal Medicine physicians and from nursing, respiratory therapy, allied health (including social work, physiotherapy) and pharmacy – all providing critical care in spaces outside of the ICU.
“Since wave two, beyond our normal patient admissions, an additional, over 150 patients with COVID were transferred to Mount Sinai and were cared for here, which helped other hospitals who were dealing with surge and over-capacity. This took a tremendous amount of nimble transformation, energy and leadership, supported by all of our dedicated clinical teams and utilization specialists and the Admitting Department Bed Board team,” says Carolyn.
“We also saw unique collaborations and were very grateful when the Hospital for Sick Children opened an adult ICU, and nurses from Women’s College Hospital joined us to be trained in our ICU in the PACU space, and support our teams there,” adds Lisa.
In the community, infection is going down, as are hospital admissions. Carolyn notes that the teams remain ready in the event of a return to increased activity, and are starting the gradual return to other hospital services.
“All of this patient care work is vital, and there is more ahead of us. We are carefully ramping up surgical and other clinical activity, and pushing forward to meet substantial patient need,” says Lisa.