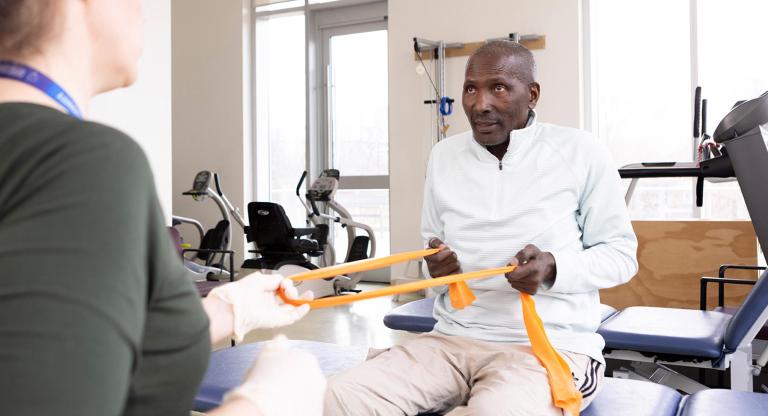
Supporting Indigenous patients in navigating the cancer care journey

Leonard Benoit starts each day with a personal smudging ceremony. Before he goes to work, he wafts the smoke of burning sage over himself, his glasses, jewelry and hospital identification badge.
Smudging is a common spiritual practice for many Indigenous peoples of North America. The smoke of one or more of the four sacred medicines—sage, sweetgrass, cedar and tobacco—is used to cleanse, dispel negativity and bring positivity.
A nurse by profession, Leonard is Qalipu Mi’kmaq from Burgeo, Newfoundland and Labrador. He is the Indigenous Patient Navigator for the Toronto Central Regional Cancer Program. He provides support for patients going through cancer treatment at seven hospital sites, including Bridgepoint Active Healthcare and Mount Sinai Hospital. Leonard frequently provides navigation assistance to patients coming to Toronto from other parts of the province to receive cancer care.
One of Leonard’s roles is to help make it easier for Indigenous patients to access spiritual practices such as smudging, pipe ceremonies, drumming and singing during their care journey.
Leonard often works closely with the Spiritual Care team at Sinai Health to arrange these ceremonies, which look different for different patients. One patient may wish to access smudging as part of their regular spiritual practice during a hospital stay. Another patient may want to hold a smudging ceremony at the beginning of chemotherapy treatment. Patients also request smudging at end of life, a tradition that helps the person make the transition from this world to the next.
Incorporating these traditions is an example of providing culturally responsive care for Indigenous patients. “This is care that honours who the patient is as a person,” says Leonard.
In order to provide truly culturally responsive care, Leonard says it’s also essential for health care providers to gain a better understanding of the lived experiences of Indigenous people in Canada. “Clinicians need to hear the true narrative of Canada they may not have learned in school,” he says.
Through education sessions, Leonard teaches clinicians about the history of residential schools and other attempts to assimilate Indigenous people and erase Indigenous cultures and identities. He discusses how the trauma from these policies has been passed down through generations.
Leonard also talks about how systemic racism continues to affect Indigenous people today and how that impacts equitable access to care. “As an Indigenous person, I may live around the corner from a hospital, but what if I have had a negative experience with health care in the past? How do I know that I will feel safe and be treated with dignity? If I do experience racism, what can I do about it? I ask these types of questions to plant seeds in peoples’ minds to help them see things from the perspective of the patient, to better understand where they’re coming from.”

As an advocate, Leonard hopes he can help further remove barriers to access a truly culturally responsive care experience for Indigenous patients. “The health care system was not designed for Indigenous folks,” says Leonard. “So it has to be adapted.”
Leonard has a wish list of actions he’d like to see. For clinicians, he would like more opportunities to learn about Indigenous history and the challenges accessing care as well as more training in trauma-informed care. For patients, he would like to see better access to elders and traditional knowledge keepers for Indigenous patients in the hospital as well as dedicated wellness spaces for Indigenous spiritual practices. Finally, he’d like to see more Indigenous Patient Navigators to support Indigenous patients and their families.
Patients and families can contact Leonard Benoit, Indigenous Patient Navigator for support during their cancer care journey and for access to smudging and other ceremonies. Health care professionals can also reach out on behalf of cancer patients who have self-identified as Indigenous, with the permission of the patient. Leonard Benoit can be reached at [email protected].