“I wasn’t ready to give up” – How teams of experts at Sinai Health, UHN and SickKids came together to save a woman and her baby
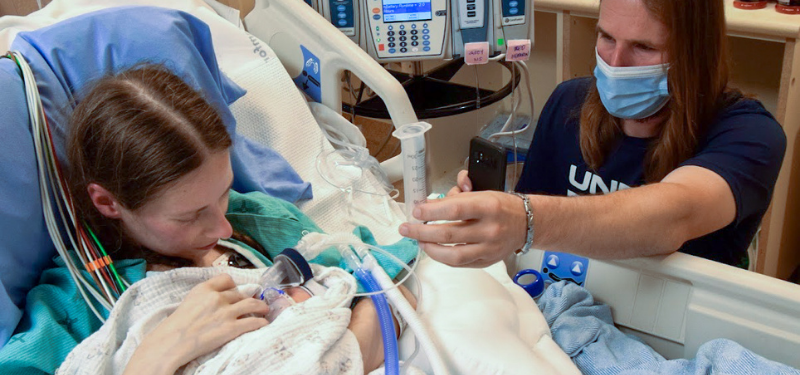
Candice Cruise was 21 weeks pregnant when, driving home one day with her husband, Collin, she noticed in the mirror of the car’s sun visor that her lips had turned blue. She had been feeling a bit out of breath on recent days, but had dismissed it as something common during pregnancy.
The couple decided to go to the local hospital and get Candice checked.
“It all happened so fast,” Candice recalls. “When I look back, it scares me to think what would have happened if we didn’t seek help that day.”
Candice and Collin could never imagine what lay ahead. There was a fight against a deadly condition for mother and baby; support by a world-first innovation and the dedication of medical teams at three Toronto hospitals; open-chest surgeries, pre-term delivery and lung transplantation.
When Candice arrived at her local hospital last April, her oxygenation was so low that the doctors quickly transferred her to Toronto’s Mount Sinai Hospital, part of Sinai Health, and the reference centre for high-risk obstetrics.
Shortly after arriving there, the medical team made the call to transfer Candice to Toronto General Hospital for evaluation of a possible devastating heart-lung condition known as pulmonary hypertension, a life-threatening disorder that leads to the narrowing of the arteries in the lungs. UHN has a comprehensive pulmonary hypertension program and is the provincial lead for extracorporeal membrane oxygenation (ECMO) – a last resource for patients with acute respiratory and circulatory failures.
After confirming the diagnosis of pulmonary hypertension, Candice’s condition began to become unstable. A quick decision was required to stabilize her and she was placed on ECMO.
“At that time, doctors told us, unfortunately, that it would be safest to terminate the pregnancy to keep Candice alive,” Collin recalls.
However, as Candice stabilized in the hours and days that followed, medical leads from Mount Sinai, UHN and The Hospital for Sick Children (SickKids), started to ask themselves if anything could be done to save both, mother and baby.
“I could feel the baby moving inside me, so strong. I knew there was nothing wrong with him, and I felt he had a good chance,” says Candice. “I wasn’t ready to give up.”
A life-threatening condition
“In a complex case like Candice’s, difficult choices need to be made that balance the risks to the mother with the health of the developing baby,” says Dr. John Snelgrove, maternal-fetal medicine obstetrician at Mount Sinai Hospital who supported Candice’s care.
Most experts recommend that patients with pulmonary hypertension avoid pregnancy given the high risk of death for the mother and her baby. However, Candice was unaware of her condition before she reached 21 weeks of pregnancy.
“We had never seen a case like this,” says Dr. John Granton, respirologist, intensive care physician and Director of the Pulmonary Hypertension Program at UHN. “Pulmonary hypertension is a dangerous condition, even more so for pregnant women, with a high risk of death for both mother and fetus.”
An ingenious plan
Experts from Obstetrics at Mount Sinai Hospital, different programs at UHN, with support from Neonatal Care at SickKids, developed an ingenious plan to keep Candice stable and buy her pregnancy a few more weeks, giving the developing baby the best chance at life.
The solution was to use an adaptable ECMO system called Novalung – a low resistance membrane that works as an external artificial lung, able to support the heart while also allowing it to continue to pump.
There were, however, complications along the way. Candice required close monitoring, adjustments to the ECMO settings and some surgical interventions.
“As this was a world-first, we didn’t have any literature to guide us. We had to use all the expertise of our teams to make clinical decisions that we hoped would achieve the best possible outcome,” says Dr. Laura Donahoe, thoracic surgeon with UHN’s Sprott Department of Surgery.
The partnership with Mount Sinai was key to push the envelope and provide Candice the best possible care.
“The NovaLung presented a novel strategy to support Candice’s heart long enough to carry her pregnancy into the third trimester,” he adds. “This is a remarkable medical success, but by far the most amazing part of this story is how courageously Candice persevered, and how dependably Collin supported her during those challenging weeks.”
Delivery
At 28 weeks and six days into the pregnancy, Candice remembers the moment she and her care team decided it was time.
Candice was going to be taken to the operating room at Toronto General for her C-section – something extremely rare as the hospital does not have an Obstetrics Department. But Candice needed to be fully monitored by ECMO experts during her delivery, as she was still being supported by the artificial lung system.
“It was so inspiring to see doctors, nurses, and respiratory therapists from these three hospitals come together on such short notice and work cooperatively as one big team,” remembers Dr. Snelgrove.
“Everybody in the OR played a vital role in the safety of Candice and her baby that day.”
While the other teams were caring for Candice, SickKids’ highly-skilled Acute Care Transport Service (ACTS) team was readying for every possible scenario to support Cameron and transfer him to the neonatal intensive care unit (NICU) at SickKids.
Once Cameron was ready, he was transferred to the NICU at St. Michael’s Hospital of Unity Health Toronto until he was discharged home.
Transplant
While preemie baby Cameron was recovering, Candice wasn’t yet out of the woods.
Her condition plus the pregnancy had put a lot of pressure on her heart. Once it became clear that she was not going to improve with medication alone, she was urgently listed for a double-lung transplant. Around a month later, she got her transplant.
With treatment, Candice got better each passing day and her new lungs adjusted to her body. She went home in August. Baby Cameron came home shortly after, in early September.
It takes a village
Candice stayed at Toronto General’s Intensive Care unit for more than four months. She and Collin say they only got through such a long difficult journey because of the support from friends, family, and especially from members of Mount Sinai Hospital, UHN, SickKids and St. Michael’s.
“I am just so grateful to all the doctors, nurses, physiotherapists, the whole team. They really were like a second family to me,” says Candice. “I’ll never forget any of them.”
This story has been edited for length. See the original story here.












