Managing diabetes in the time of COVID-19

Individuals with diabetes are at increased risk for bacterial, parasitic and viral infections.
New research from Dr. Daniel Drucker, senior scientist at Sinai Health’s Lunenfeld-Tanenbaum Research Institute, highlights how COVID-19 and Type 2 diabetes may require new approaches in treatment for hospitalized patients.
The study, “Coronavirus infections and type 2 diabetes-shared pathways with therapeutic implications,” was published online, ahead of print. Below, Dr. Drucker addresses some of the most pressing questions about managing diabetes during the COVID-19 pandemic.
Why should we focus on people with diabetes and obesity in the context of COVID-19?
We know from reports in many countries that people with Type 2 diabetes and obesity may have higher rates of hospitalization with COVID-19 infection, and a greater risk of more severe illness. So we need to be extra vigilant about measures like hand-washing, physical distancing, isolation and hygiene to prevent infection.
What about the medications for diabetes? Do they need special adjustment?
At times of severe stress, infections or illness prompting hospitalization, blood sugar might rise in some people, and adjustment of medications may be needed. More frequent monitoring of blood glucose, and checking for ketones may be advisable, depending on your own health status and advice of your diabetes health-care provider.
Is someone with Type 1 diabetes at special risk?
There is no evidence at this point that people with Type 1 diabetes have a greater risk of COVID-19 infection. Regular monitoring of glucose values, ketones, and insulin requirements should continue.
Are some diabetes medicines better than others at fighting the virus?
At this time, there is no rigorous scientific data from studies in people that highlights either a special benefit or a risk of a different outcome with COVID-19 for any of the common glucose-lowering medicines used to treat Type 2 diabetes.
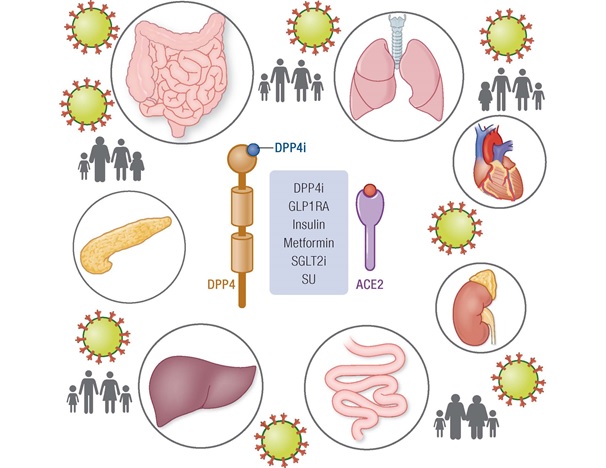
Is DPP4 not a coronavirus receptor? What about DPP4 inhibitor drugs like the gliptins?
Dipeptidyl Peptidase-4 (DPP4) is a glucose-regulating enzyme that also serves as a receptor for Middle Eastern Respiratory Syndrome (MERS) infection, a related but distinct coronavirus infection. There is no evidence that DPP4 is a receptor for COVID-19. Moreover, medications such as sitagliptin, linagliptin, saxagliptin and alogliptin, the “gliptins,” have not been shown to pose any special risk to immune function in people with diabetes, with or without infections.
What about diabetes management in the hospital?
Individuals with diabetes who may have trouble eating or drinking due to illness should check their blood sugar more frequently and contact their health-care provider. People who are admitted to hospital may need to have their diabetes medications reassessed. Some people may need medication dose adjustments, in other cases some medications may be stopped. It is important to seek medical advice if you have diabetes and think you might have COVID-19.












