Mount Sinai’s ICU plans for the future of intensive care
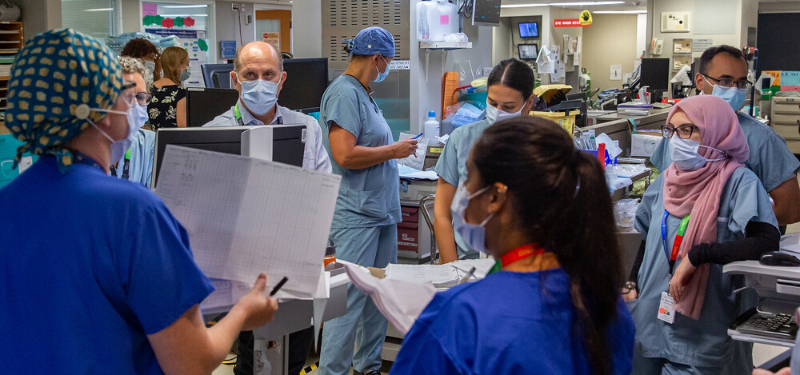
Just prior to the World Health Organization declaring that COVID-19 had reached the threshold of a global pandemic, teams across Sinai Health were preparing for the need to more than double the number of beds dedicated to intensive care.
This work was done swiftly, in order to handle a possible surge of patients suffering from the worst effects of the illness to be admitted into Mount Sinai Hospital.
“We were watching the news and seeing what was happening in China, in Italy, then New York, as our teams were planning the increase in ICU beds. We knew we needed to act fast,” says Dr. Stephen Lapinsky, Director of the Intensive Care Unit says
In order to enable the existing ICU space to increase their number of beds from 18 to almost 50, the team needed to consider both small, practical details as well as system-wide changes. “We needed obvious things like gurneys and monitors, and bedside tables,” Dr. Lapinsky explains. “But we also needed to work with Engineering to arrange adequate oxygen supply, Information Services to ensure bed identifications were accurate so prescriptions and food could be delivered appropriately, not to mention that the new areas were staffed with nurses, respiratory therapists, housekeepers, and many other health disciplines to serve our patients.”
“Across the hospital, we saw a rapid succession of changes in an incredibly tight timeframe. It was truly amazing to see how innovative, nimble and adaptive people were,” says Kate Van Den Broek, Senior Clinical Program Director, Urgent and Critical Care.
Thankfully, the majority of the surge beds were never needed. But the tremendous work to increase this capacity also means that should a second wave of COVID-19 happen, or even a particularly bad flu season, the hospital is in a better position to serve seriously ill patients.
“What we have now is a model that allows us to expand or contract as patient need arises,” says Kate. “This includes plans for how to staff these spaces in order to care for additional patients, Information Services infrastructure and organizational memory to get up and running quickly.”
COVID-19 has changed the landscape of care for hospitals across Canada, and the world. For the future of the ICU, this change has allowed for a better understanding of how to both respond to public health emergencies, and create patient spaces that allow for the best care while reducing the transmission of future infectious diseases.