A look back at Sinai Health’s pandemic response
Image

On April 19, health-care workers across the city were treated to an outpouring of gratitude from some of Toronto’s emergency service providers. Emergency vehicles put on their lights and sirens to celebrate the work of hospital and long-term care workers.
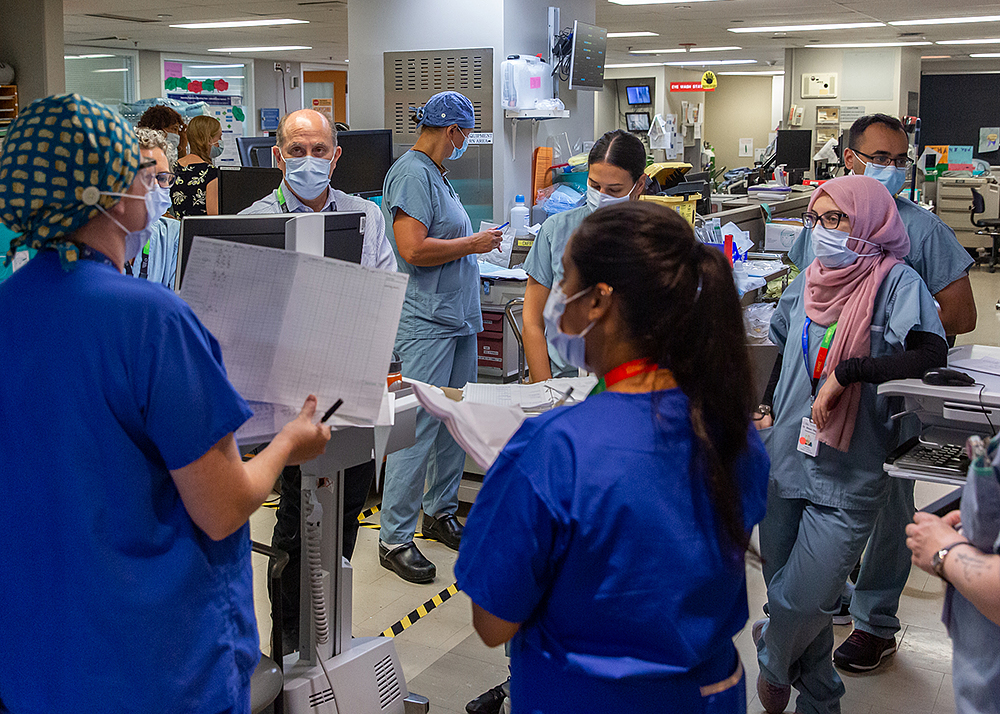
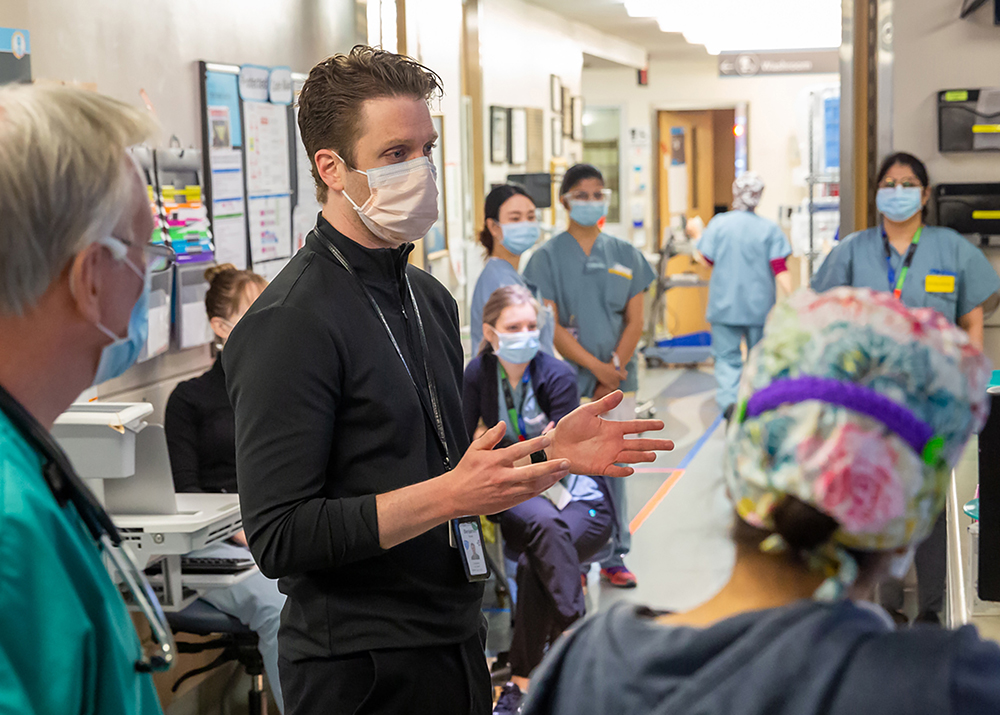
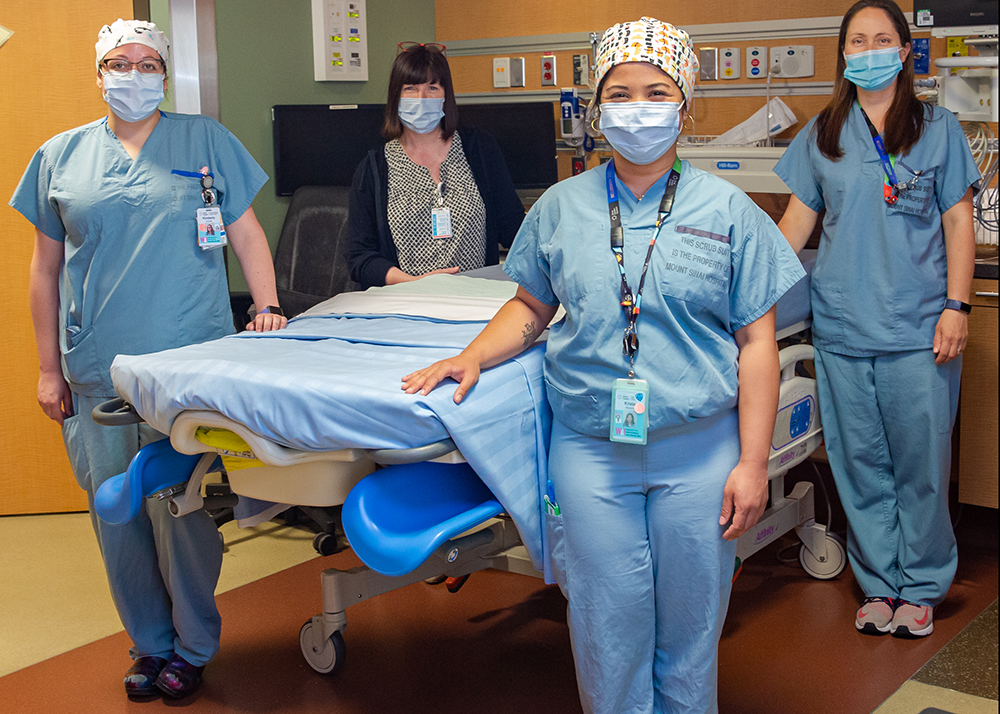
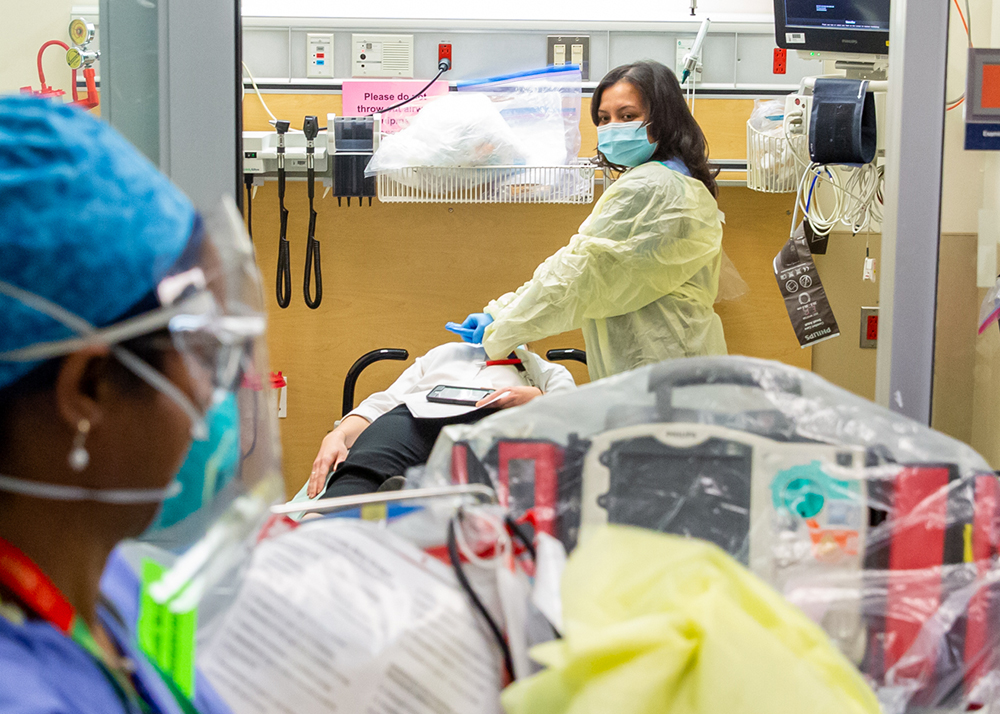
On March 11, 2020 the World Health Organization declared COVID-19 to be a global pandemic. Since then, the teams at Sinai Health have worked tirelessly to respond to the needs of our patients, community and each other.
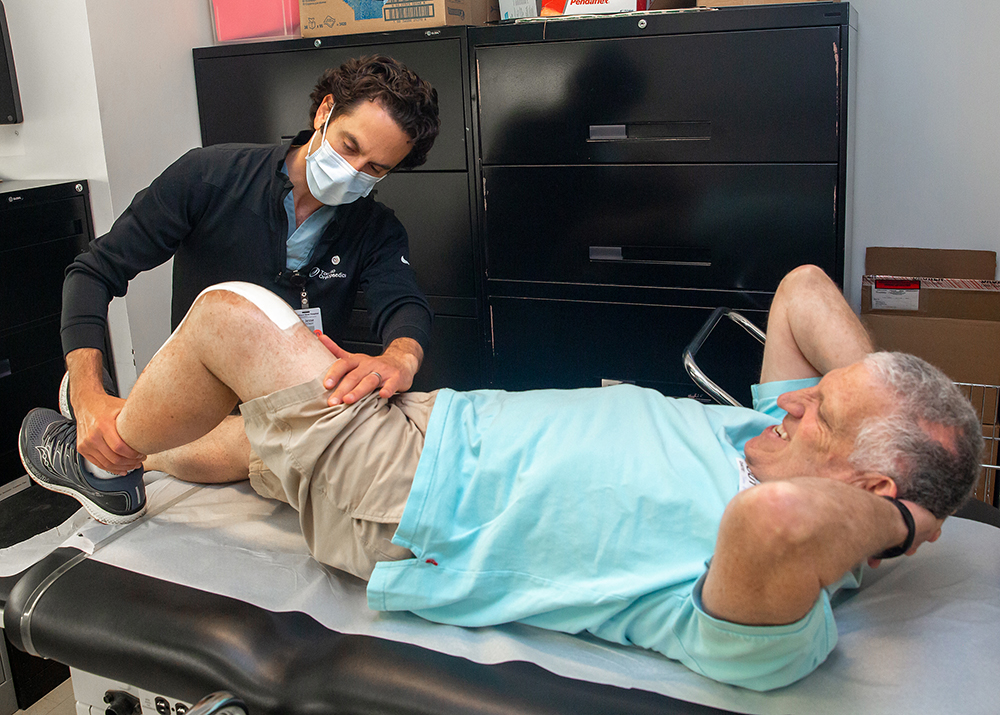
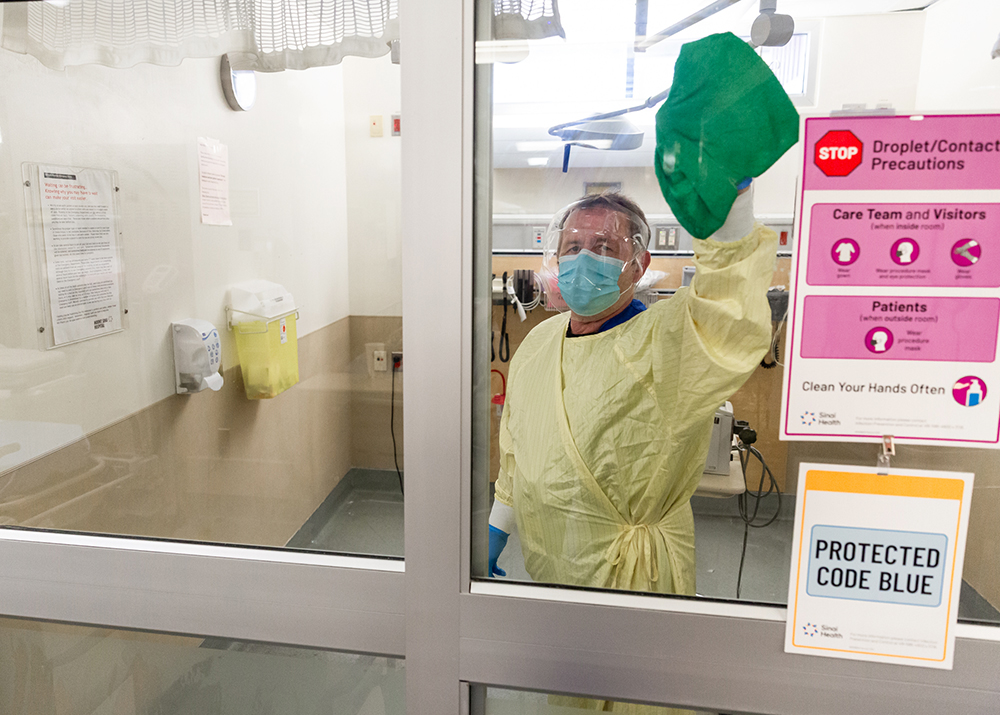
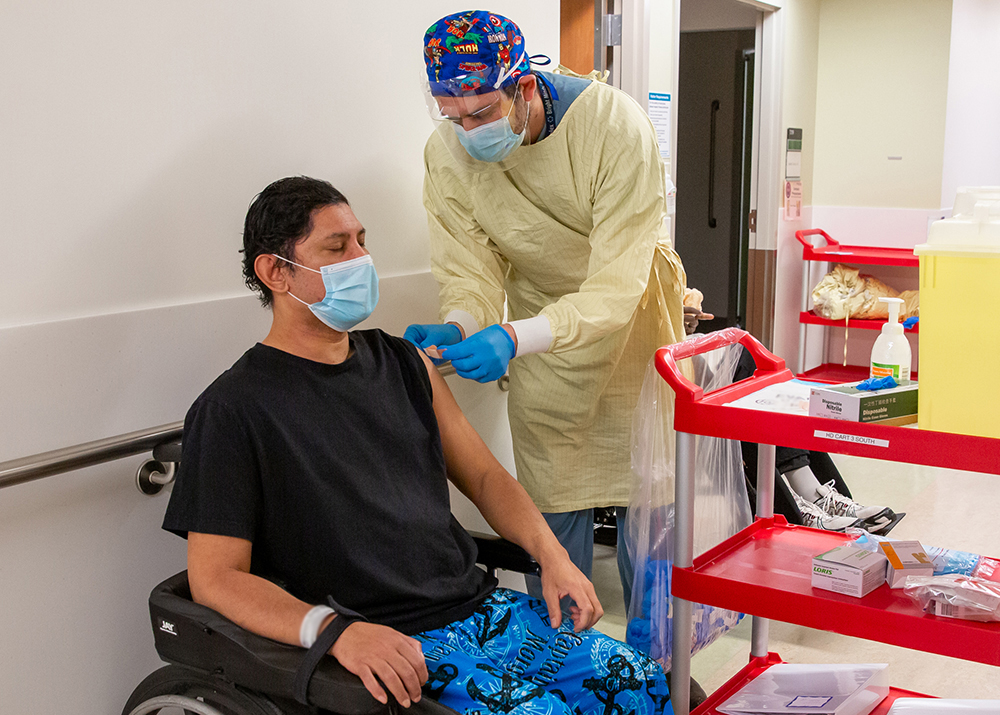
Below are some photos taken over the course of the last year that capture an inside look at how Mount Sinai Hospital, Bridgepoint Active Healthcare and Lunenfeld-Tanenbaum Research Institute have worked with dedication and compassion during a time when the only certainty was change.
Please note that photos taken over the course of the COVID-19 pandemic may not reflect the protocols now in place across Sinai Health.
Find another story: