Advancing surgical precision: How 3D innovation is improving outcomes and reducing hospital stays
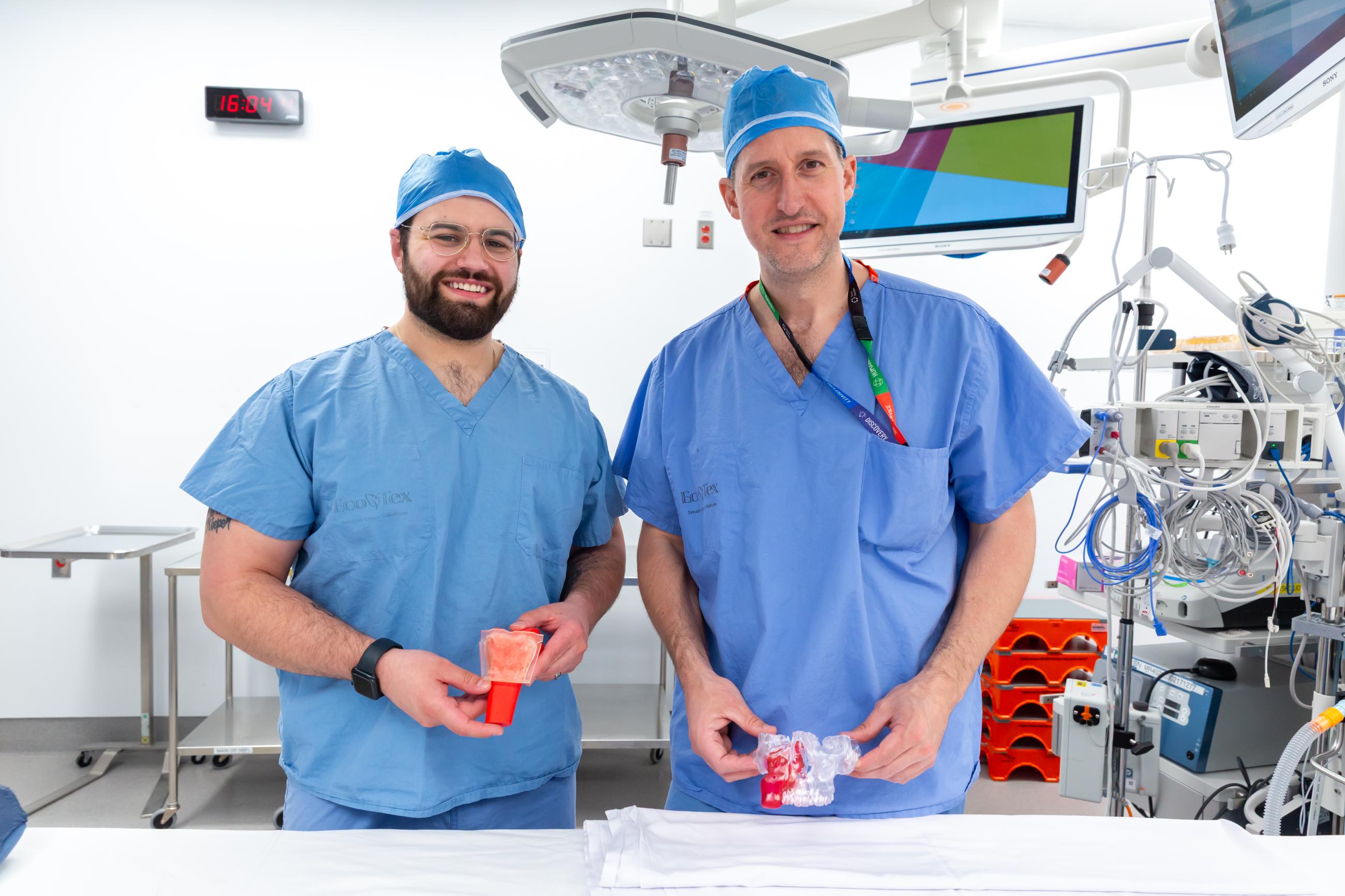
A bold investment in robotics and 3D modelling at Sinai Health is paying off. Not only in the operating room, but in faster recoveries, shorter hospital stays and improved outcomes for patients across multiple specialties.
Led by otolaryngologist Dr. Joel Davies, this work brings together surgeons, the biomedical engineering team and the medical device reprocessing department (MDRD) to integrate 3D printing and virtual surgical planning into patient care. What began as an exploration of new technology has quickly evolved into a leading-edge program, marking a milestone for surgical innovation in Canada.
Research and innovation at Sinai Health are closely tied to care delivery, with a focus on improving outcomes and experiences for patients.
Improving care through precision
Using patient-specific 3D models and custom surgical guides, teams can now plan complex tumour resections and reconstructions in advance allowing for more accurate, efficient procedures in the operating room.
“3D printing and virtual surgical planning are transforming how we approach complex cancer surgery,” said Dr. Ian Witterick, Surgeon-in-Chief at Sinai Health. “By allowing us to visualize tumours in three dimensions and plan resections and reconstructions in advance, we can operate with greater precision, reduce operative time, and ultimately achieve better outcomes for our patients. These technologies are not only enhancing care, they are also powerful tools for education and training the next generation of surgeons.”
This shift replaces a more manual and approximate approach, improving alignment during reconstruction and reducing the risk of complications.
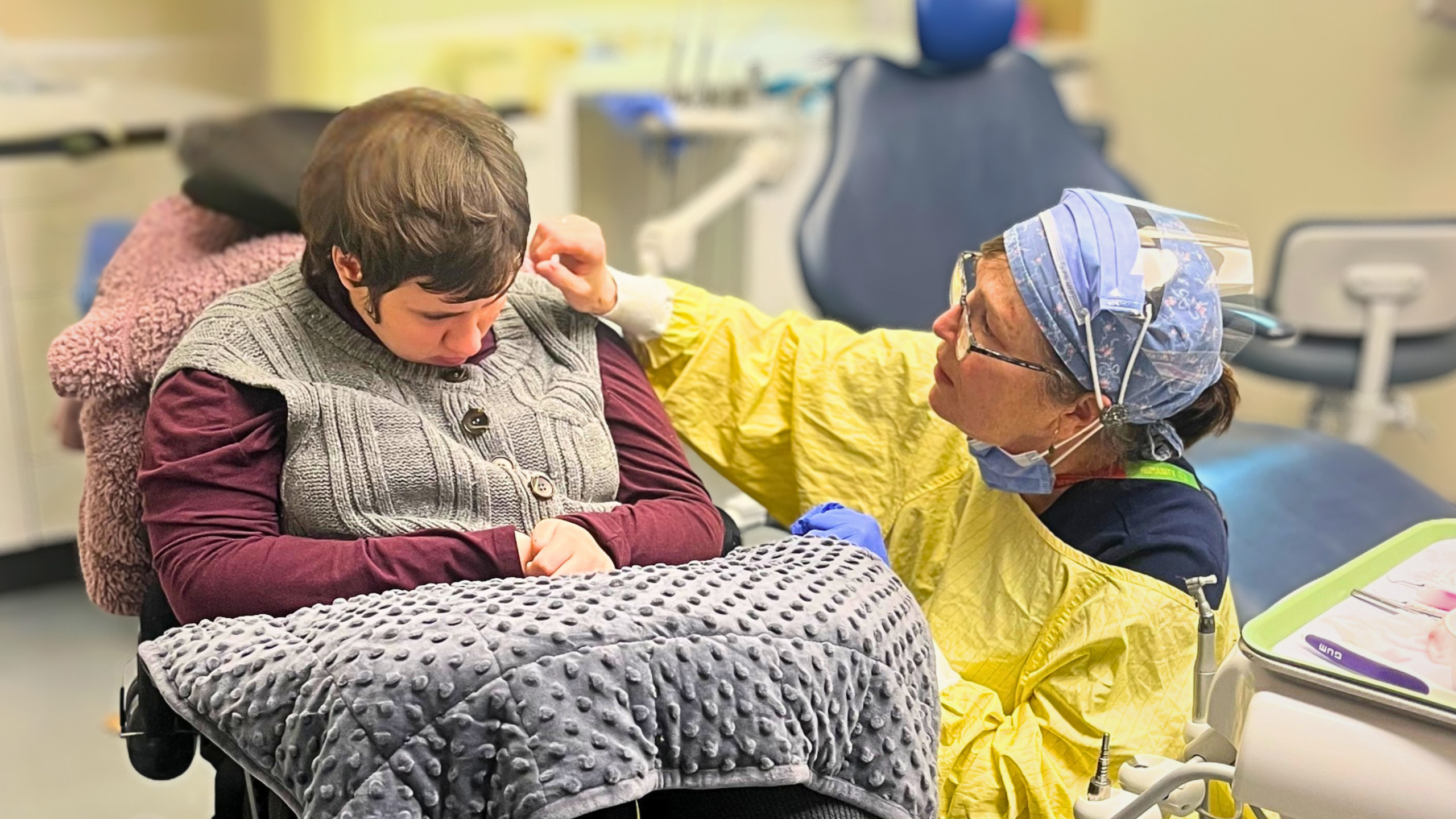
In many cases, the true size and shape of a tumour can be difficult to convey using traditional imaging alone, especially when it sits deep within soft tissue or changes gradually over time. That’s where three-dimensional models can make a real difference in helping patients understand what’s happening inside their own bodies.
“Sometimes patients don’t fully understand the extent of the tumor because it’s hidden by soft tissue, or it’s been growing slowly over time. But when they see the model, it clicks. You can point to specific areas and explain” adds Dr. Davies.

Shorter surgeries, faster recovery
Dr. Davies’ research shows the approach is saving approximately 100 minutes per surgery in many cases – a significant reduction in procedures where timing is critical.
“We’re not just improving precision, we’re fundamentally changing how these surgeries are performed. By planning in advance and executing with that level of accuracy, we’re reducing risk, improving efficiency and ultimately helping patients recover faster,” said Dr. Davies.
The benefits extend beyond the operating room. Early data shows that patients are spending, on average, three fewer days in hospital following these procedures.
Shorter lengths of stay support faster recovery for patients while also improving access to care by freeing up capacity within the system. Procedures that once extended into the evening are now often completed within standard operating hours.
Collaboration driving innovation
A key factor in the program’s success is collaboration across disciplines, with an integrated, in-house system.
The MDRD has become an essential partner in bringing 3D-printed surgical innovation into the operating room. Working hand-in-hand with the biomedical engineering and surgical teams, MDRD ensures that each custom-printed model and cutting guide is sterilized to the same rigorous standards as any surgical instrument.
The team collaborated closely with the biomedical engineering team to validate and refine the sterilization process, confirming that even the most intricate models remain structurally unchanged and fully sterile after processing. Their detailed tracking and quality assurance system means every component can be traced through each stage of preparation.
Biomedical engineer technologist Qwynn Ferreira played a central role in developing the program, applying self-directed learning and working to translate technical concepts into practical tools for patient care.
“I had to learn how to create something that was not just technically accurate, but safe and usable in a clinical setting,” he says.
The impact became clear early on, when a complex reconstruction case was completed hours faster than expected and went exactly to plan.
“That was the moment it really clicked,” he adds. “We were supporting real surgical decisions and making a difference for patients.”
Each model and guide undergoes rigorous validation, including test-fitting and quality checks. This ensures accuracy and reliability in the operating room.
A leading model in Canada
The model is already expanding into other areas, including orthopaedic oncology, and continues to evolve with new applications such as mixed reality in surgery.
What began as a calculated investment in robotics and 3D technology is now delivering measurable improvements in care - positioning Sinai Health as a leader in surgical innovation in Canada.
This work reflects Sinai Health’s broader commitment to advancing care through research, innovation and collaboration.